Every year, millions of consumers experience adverse skin reactions from cosmetic and skincare products, with contact dermatitis affecting approximately 20% of the population at some point in their lives. The rapid expansion of the beauty industry, coupled with increasingly complex formulations containing multiple active ingredients, has made patch testing more crucial than ever before. What was once considered an optional precaution has now become an essential step in maintaining skin health and preventing potentially severe allergic reactions.
Professional dermatologists and cosmetic chemists have long recognised that individual skin sensitivity varies dramatically from person to person, making it impossible to predict reactions based solely on product labelling or general safety assessments. Patch testing represents the gold standard for identifying potential allergens before they can cause widespread skin damage, offering both consumers and healthcare professionals a reliable method for preventing contact dermatitis and related inflammatory conditions.
Understanding allergic contact dermatitis and sensitisation mechanisms
Allergic contact dermatitis represents a complex immune-mediated response that develops when the skin’s immune system recognises specific chemical compounds as foreign threats. Unlike immediate allergic reactions that occur within minutes of exposure, contact dermatitis typically manifests 24 to 72 hours after initial contact with an allergen. This delayed response mechanism makes it particularly challenging to identify causative agents without systematic testing protocols.
Type IV hypersensitivity reactions in cosmetic product testing
The immune system’s response to cosmetic allergens follows a Type IV hypersensitivity pathway, also known as delayed-type hypersensitivity. This process involves T-lymphocytes rather than antibodies, creating a cellular immune response that can persist for weeks or months once sensitisation occurs. When allergens penetrate the skin barrier, they bind to proteins within the epidermis, forming hapten-protein complexes that trigger antigen-presenting cells to activate T-helper cells.
This sensitisation phase typically requires multiple exposures over time, explaining why individuals may use products successfully for months before developing sudden allergic reactions. Once sensitisation occurs, even minimal exposure to the offending allergen can trigger inflammatory responses characterised by erythema, vesicle formation, and intense pruritus.
Common allergens in skincare: fragrance molecules and preservative systems
Research conducted by the European Centre for Allergy Research Foundation indicates that fragrance components account for approximately 35% of all cosmetic-related contact dermatitis cases. The most frequently implicated compounds include cinnamaldehyde, eugenol, and hydroxycitronellal, which are commonly found in perfumes, skincare products, and household cleaning items. These molecules possess reactive functional groups that readily bind to skin proteins, facilitating the sensitisation process.
Preservative systems present another significant category of concern, with formaldehyde-releasing agents such as DMDM hydantoin and quaternium-15 leading to reactions in susceptible individuals. Methylisothiazolinone, once considered a safer alternative to parabens, has emerged as a major sensitiser, particularly in leave-on cosmetic products where prolonged skin contact increases exposure risk.
Cross-reactivity patterns between related chemical compounds
One of the most complex aspects of contact sensitisation involves cross-reactivity between chemically related compounds. Individuals sensitised to para-phenylenediamine, commonly found in hair dyes, often develop reactions to structurally similar molecules including certain sunscreen ingredients, topical anaesthetics, and textile dyes. This phenomenon extends beyond obvious chemical families, with some patients showing unexpected cross-reactions between botanically derived ingredients and synthetic compounds sharing similar molecular structures.
Understanding these cross-reactivity patterns proves essential for comprehensive allergen avoidance strategies. Professional patch testing protocols typically include multiple related compounds to identify potential cross-sensitivities that might not be apparent from single-allergen testing approaches.
Individual genetic predisposition to contact sensitisation
Recent genomic research has identified specific genetic variations that influence individual susceptibility to contact sensitisation. Polymorphisms in genes encoding cytochrome P450 enzymes, which metabolise xenobiotic compounds, can affect how efficiently the skin processes potential allergens. Additionally, variations in genes
involved in skin barrier formation, such as filaggrin (FLG), have been strongly associated with increased rates of allergic contact dermatitis and atopic eczema. When the barrier is inherently weaker, small reactive molecules penetrate more easily, increasing the likelihood that they will bind to skin proteins and trigger the immune cascade described earlier. This helps explain why some people seem to “react to everything,” while others can tolerate fragranced and highly active formulations without visible irritation. Understanding your own predisposition is therefore a key part of deciding how strict you should be with patch testing before trying new products.
Professional patch testing protocols and clinical standards
When adverse reactions become persistent, severe, or difficult to explain, professional patch testing in a dermatology clinic becomes essential. Unlike simple at-home patch tests, clinical protocols use standardised allergen mixes, controlled application methods, and validated scoring systems. This allows dermatologists to differentiate between true allergic contact dermatitis, irritant reactions, and non-specific sensitivity, giving you a clear roadmap for safe skincare choices going forward.
European standard series testing with TRUE test panels
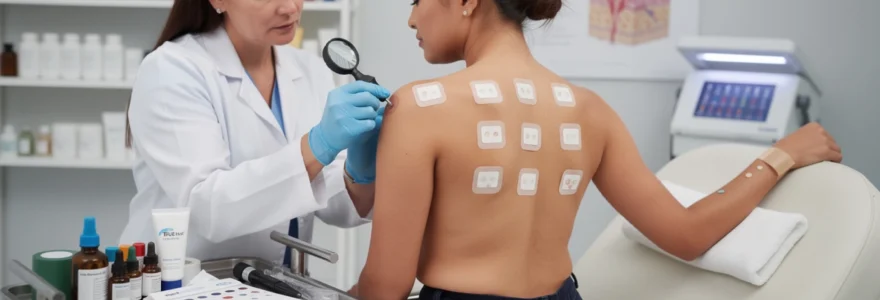
In many regions, particularly across Europe and North America, dermatologists rely on the European baseline series of allergens, often applied using pre-prepared TRUE Test (Thin-layer Rapid Use Epicutaneous) panels. Each panel contains a fixed set of common sensitising substances embedded in a gel on small discs, which are then applied to the back using hypoallergenic adhesive tape. This standardisation ensures that the concentrations, exposure times, and placement are consistent from one patient to another, improving the reliability of patch test results.
Depending on your history and occupation, your dermatologist may add extra panels for cosmetics, hairdressing chemicals, rubber accelerators, metals, or fragrances. For example, someone reacting to multiple skincare products may be tested not only with common preservatives and fragrance mixes, but also with their own creams or serums diluted to safe concentrations. Have you ever wondered why one product gives you a rash while a very similar one does not? Comprehensive professional patch testing with expanded series often reveals subtle differences in formulation that explain these confusing patterns.
48-hour and 72-hour reading intervals for accurate results
Standard patch test protocols usually involve applying the panels and leaving them in place for 48 hours, during which you must keep the area dry and avoid heavy sweating. At the first reading, around the 48-hour mark, the dermatologist removes the panels and inspects the skin for early signs of reaction. However, because Type IV hypersensitivity is delayed, many clinically relevant reactions only become clear at the second reading, typically around 72 to 96 hours after application.
This two-stage assessment helps to distinguish between transient irritation from occlusion or pressure and genuine allergic responses that continue to evolve after the allergens are removed. It can feel a bit like waiting for film to develop: the initial image appears at 48 hours, but the full picture of your sensitivity profile only comes into focus over the next day or two. For this reason, skipping the later reading can result in missed diagnoses or underestimation of your skin’s reactivity to certain cosmetic ingredients.
ICDRG scoring system for reaction assessment
To ensure consistency between clinics and practitioners, patch test reactions are interpreted using the ICDRG (International Contact Dermatitis Research Group) scoring system. Rather than simply labeling a site as “positive” or “negative,” dermatologists grade the intensity and morphology of the reaction on a scale, from doubtful or irritant (+/IR) through weak positive (+), strong positive (++), and extreme positive (+++). Each grade reflects specific visual signs such as erythema, papules, vesicles, or even blistering at the test site.
Why does this level of detail matter for you as a skincare consumer? Because a weak, borderline reaction to a preservative might mean you can still use rinse-off products containing small amounts of it, while a strong or extreme reaction usually indicates you should avoid that ingredient category altogether. The ICDRG system also helps to identify false positives caused by mechanical irritation or tape allergy, ensuring that you are not unnecessarily restricting your choice of cosmetic and personal care products.
Photopatch testing for UV-Activated allergens
Some individuals only react to a substance when it is combined with ultraviolet (UV) exposure, a phenomenon known as photoallergic or phototoxic contact dermatitis. Sunscreens, certain fragrances, and specific topical medications can become problematic only when your skin is exposed to sunlight after application. To investigate these UV-activated allergens, dermatologists may perform photopatch testing, which adds an extra step to the standard protocol.
In photopatch testing, two identical sets of potential photoallergens are applied to the back. After 48 hours, one set is removed and exposed to a controlled dose of UVA light, while the other remains covered as a control. Both sites are then evaluated 24 to 48 hours later. If a reaction appears only on the irradiated side, this strongly suggests a photoallergic mechanism. For anyone who repeatedly develops rashes on sun-exposed areas after using new sunscreens or “day creams,” photopatch testing can be the missing piece that finally connects the dots.
Consumer-grade patch testing methodologies for home use
While professional patch testing remains the diagnostic gold standard, most consumers will first rely on simple at-home methods before visiting a dermatologist. Properly performed, home patch testing can significantly reduce the risk of widespread reactions from new skincare, haircare, or cosmetic products. The key is to mimic, as far as possible, the controlled exposure and observation used in clinical settings, while adapting the procedure to everyday life.
24-hour elbow crease testing protocol
One of the most practical at-home techniques is the 24-hour elbow crease test, which uses the inner bend of your arm as a proxy for more sensitive areas such as the face or neck. This region has relatively thin skin and experiences some natural friction, offering a realistic picture of how your skin might respond in daily use. To perform the test, you apply a small amount of the product—about the size of a pea—to a quarter-sized area within the elbow crease, then leave it undisturbed for at least 24 hours.
During this period, you should avoid washing or heavily rubbing the area, and you should not layer other products on top. If you are testing a cleanser or rinse-off mask, leave it on for the amount of time recommended on the label (usually a few minutes), then rinse gently and observe the area over the next day. Mild, transient tingling—particularly with exfoliating acids—may be acceptable, but persistent burning, pronounced redness, or swelling are clear signs that the product may not be suitable for full-area application.
Behind-the-ear application for facial product assessment
For products specifically intended for facial use, such as serums, moisturisers, or sunscreens, applying a small amount behind the ear can provide especially relevant information. The skin in this region closely resembles facial skin in thickness and sensitivity, yet it is discreet enough that any reaction will be easily concealed. You can place a thin layer of the product just behind the earlobe once or twice a day for two to three days, mirroring how you intend to use it on your face.
Have you ever been tempted to slather a new active serum all over your face after reading glowing reviews? By taking the simple step of testing behind the ear first, you give your skin a chance to “vote” on the product in a controlled way. If, after 48 to 72 hours, there is no itching, redness, or flaking, you can proceed with more confidence to cautious full-face use. Conversely, if even this small area reacts, the behind-the-ear patch test will have spared you from a potentially uncomfortable or embarrassing reaction.
Graduated introduction method for multiple ingredient products
Modern skincare formulations often contain complex blends of actives, humectants, fragrances, and preservatives. This makes it difficult to know which specific component is responsible when your skin reacts. To reduce this uncertainty and minimise the risk of overwhelming a sensitive skin barrier, a graduated introduction method is recommended. Instead of adding several new products at once, you introduce them one at a time, with a gap of several days between each new addition.
In practice, this might mean patch testing a new moisturiser for a week, then gradually applying it to the full face every other day, before introducing a new serum or exfoliant. Think of this like building a house: you lay one solid brick at a time, checking its stability before adding the next. This method not only makes it easier to identify the culprit if a reaction occurs, but it also gives your skin time to adapt to new ingredients and reduces the risk of cumulative irritation from multiple actives used together.
Documentation and photography techniques for reaction monitoring
When you are testing new products at home—especially if you have a history of sensitive or reactive skin—systematic documentation can be surprisingly helpful. Subtle changes such as mild redness, small bumps, or tightness can be easy to dismiss in the moment but become significant when viewed over time. Taking clear photographs of your test area at baseline, 24 hours, and 72 hours after application allows you to track progression and provides valuable evidence if you later consult a dermatologist.
To keep this simple, you can use your smartphone and take photos in consistent lighting conditions, ideally near a window with natural light. Note down the product name, ingredients list, date of first use, and any symptoms you notice, such as itching or burning. This process turns your at-home patch testing into a mini “skincare lab,” enabling you to make more objective decisions rather than relying solely on how you feel in the moment. Over time, patterns will emerge that highlight which ingredient types your skin tends to love—and which it would rather avoid.
High-risk product categories requiring mandatory testing
Not all cosmetic products carry the same risk of triggering allergic contact dermatitis or irritation. Certain categories are inherently higher risk and should almost always be patch tested before regular use, especially if you have a known history of sensitive skin or eczema. Leave-on products with high concentrations of active ingredients—such as retinoids, chemical exfoliants (AHAs and BHAs), and potent vitamin C serums—are prime examples, as they remain in prolonged contact with the skin and directly influence barrier function.
Fragranced body lotions, perfumed deodorants, hair dyes, and nail products also fall into the high-risk group due to their frequent association with fragrance and preservative allergies. Similarly, “long-wear” or “waterproof” formulations often rely on more robust film-forming agents and solvents, which can be problematic for some individuals. By treating these formulations as requiring mandatory patch testing before trying new products on a larger area, you dramatically reduce the chance of developing a severe or widespread reaction that is difficult to calm.
Interpreting patch test results and false positive indicators
Whether testing at home or in a clinic, understanding how to interpret patch test results is crucial. A clear, bright-red area that itches or burns and persists beyond a day usually indicates a true reaction, particularly if it is well defined and corresponds exactly to the application site. In contrast, faint redness that fades quickly, or slight dryness without discomfort, may simply reflect temporary irritation or the skin adjusting to an active ingredient like glycolic acid or retinol.
False positives are an important consideration. For example, leaving an occlusive plaster on for too long can itself cause redness or maceration, especially in warm, sweaty conditions. Similarly, highly concentrated products applied under occlusion can provoke irritant reactions even in non-sensitive individuals, which may be mistaken for allergy. To minimise misinterpretation, you should compare the tested area to nearby untreated skin and consider the overall pattern of symptoms. When in doubt—particularly after a severe or blistering reaction—seeking professional evaluation will help you avoid unnecessary long-term avoidance of ingredients that may not truly be problematic.
Post-reaction management and dermatological intervention strategies
Despite careful patch testing, reactions can still occur, especially when dealing with highly sensitised or compromised skin. Prompt, appropriate management is key to limiting discomfort and preventing longer-term issues such as post-inflammatory hyperpigmentation or chronic eczema. The first step is always to remove the offending product and gently cleanse the area with lukewarm water and a bland, fragrance-free cleanser, avoiding scrubbing or harsh towels.
For mild reactions, cool compresses and the application of a simple, fragrance-free emollient or petroleum jelly can provide soothing relief and support barrier repair. Over-the-counter topical corticosteroids may be appropriate for short-term use in some cases, but you should consult a healthcare professional before applying them to sensitive areas like the face or eyelids. If you experience severe swelling, intense burning, blistering, or symptoms that spread beyond the application site, seeking prompt dermatological assessment is essential, as stronger prescription treatments or even systemic medications may be required.
In a clinical setting, dermatologists will not only treat the active reaction but also help you build a long-term prevention strategy. This may include formal patch or photopatch testing, the creation of a personalised “safe list” of ingredients and brands, and education on how to read ingredient labels effectively. Over time, this combination of careful product selection, consistent patch testing before trying new products, and timely professional guidance can transform a frustrating cycle of trial-and-error into a calm, predictable skincare routine that supports both the health and comfort of your skin.